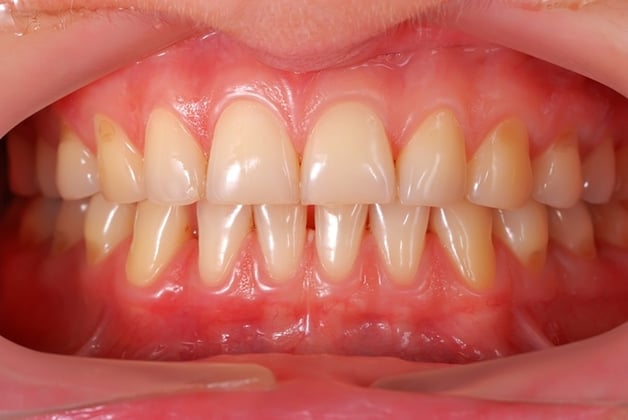
Periodontal disease, otherwise known as gum disease, surfaces in many forms. For example, with the first stage of this condition, called gingivitis, you may notice only slightly swollen or irritated gums and, fortunately, it can be reversed. Full blown periodontitis, on the other hand, is marked by bleeding, puffy and bright red gums often accompanied by gingival recession, that is, a receding gum line. Gingival recessions bring on a new slew of complications for oral health.
"If plaque is not brushed away, it destroys the gums."
What is gingival recession?
Periodontitis leads to gingival recession when plaque and bacteria stretch down the surface of the tooth. If the plaque is not brushed away, it irritates and destroys gum tissue, forcing the gums to detach from the tooth.1 Once this happens, the problem is only worsened as more bacteria collect in the pockets of space between the teeth and the gums, allowing gingival recession to progress even further.
Diagnosing gingival recession
Depending on the severity of your gingival recession, the receding gum line might be visually apparent. Since gingival recession typically isn't a drastic or immediate change, you may need to utilize other clues to spot this condition. For example, your tooth may appear longer than normal or your gums may bleed more easily. During gingival recession's latest stages, your may experience loose teeth and exposed roots.
Your dentist may be able to spot these visual cues before they worsen, or he or she may use a process called probing to determine whether you have gingival recession. A periodontal probe is a diagnostic tool that measures the depth of those pockets formed when the gum pulls away from the tooth. Healthy gums usually have pocket depths of only 1-3 millimeters.2 Measurements outside that range may indicate gingival recession.
Your dentist will suggest certain oral care changes, such as using a toothbrush with softer bristles, and he or she may refer you to a gum specialist, called a periodontist, who can outline a more extensive treatment plan.

The type of toothbrush you use may play a role in gingival recession.
Gingival recession causes
Though gingival recession usually stems from periodontitis and overall poor oral health, there are a number of other factors that can also contribute to its development. For example, aggressively brushing your teeth, using a hard-bristled toothbrush or frequently using horizontal motions can cause the gum line to recede. Fortunately, this problem is easily corrected by switching to safer oral hygiene habits.
Not as easily amendable, misaligned teeth may also cause gingival recession.3 When a tooth is not in a correct position, the gum is pulled in an unnatural way and is thus more susceptible to recession. What's more, it may be harder to clean abnormally positioned teeth, and poor oral health causes this gum condition.
Teeth grinding, otherwise known as bruxism, could lead to gingival recession. First, the sheer pressure of clenching your jaw pushes down the gum line. What's more, moving the jaw in a back-and-forth motion throughout the night can loosen teeth and form gum pockets.
Oral health complications
Your gums are supposed to keep your teeth in place and protect them. When the gum line recedes and the root is exposed, you may experience greater sensitivity, which can make even brushing your teeth a painful experience. Of course, you can treat sensitivity with certain oral care products, such as desensitizing tooth paste, but that will provide only temporary relief.
Gingival recession can also make you more susceptible to decay, as the root is not protected by enamel, the hard surface that covers other areas of your teeth.4 A combination of cavities and unsupported teeth can lead to tooth loss as well.
"Once the gum tissue is gone, it cannot come back."
Treatment options
Once the gum tissue is gone, it cannot come back. Treatment plans for gingival recession target prevention and include incorporating healthier habits into your dental routine and avoiding brushing too hard. However, if the gum line has severely receded, surgery may be required - you and your periodontist will make that decision together.
Flap surgery refers to when the periodontist cuts the gum with a scalpel and pulls the flap back, hence the procedure's name. This exposes the entire tooth surface and allows the dental health professional to thoroughly clean the area, removing any plaque or inflamed tissue. The periodontist will also correct any possible bone defects beneath the gums' surface. The periodontist then replaces the tissue, often allowing it to reach higher on the tooth to correct the recession, and stitches it in place.
When not enough gum tissue is present to fold back and clean under, the periodontist may choose to perform a graft surgery to replace the receding gum line. During gum graft surgery, the dental health professional removes healthy tissue from an unaffected area, such as the roof of the mouth, palate or an adjacent tooth.5 He or she then scraps off the backside of that tissue and uses it to cover the exposed roots. The periodontist replaces the remaining tissue to its original position.
Preventing gingival recession
While there are a number of treatment options available, it's best to avoid gingival recession altogether. Practice proper oral care by gently brushing your teeth twice a day with a soft-bristled toothbrush and flossing once a day. It's also crucial to visit the dentist at least twice per year, but additional appointments may be necessary if you spot the early signs of a receding gum line. You may benefit from utilizing a low cost dental care plan with the help of a dental discount card.
______________________________________________________________
1. "Receding Gums," California Dental Association. http://www.cda.org/Portals/0/pdfs/fact_sheets/receding_gums_english.pdf
2. "Periodontal (Gum) Disease: Causes, Symptoms, and Treatments," National Institutes of Health, Sept. 2013. http://www.nidcr.nih.gov/OralHealth/Topics/GumDiseases/PeriodontalGumDisease.htm
3. "Receding Gums And Treatment And Causes," Rebecca Gatesman, Colgate. http://www.colgate.com/en/us/oc/oral-health/conditions/gum-disease/article/sw-281474979262118
4. "Gum Recession Can Affect Even Healthy Mouths," Colgate. http://www.colgate.com/en/us/oc/oral-health/conditions/gum-disease/article/ada-10-gum-recession
5. "Gum Grafting," Michael C. Stypula, DDS. http://www.pittsburgh-periodontist.com/Treatments/GumGrafting.aspx
